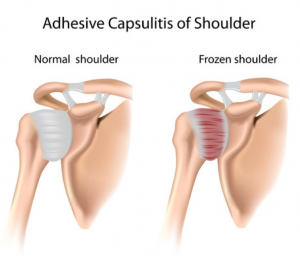
In this edition of ‘TIC Spotlight’ we take a closer look at one of the most misunderstood and often frustrating conditions of the shoulder “Frozen Shoulder” or to give it it’s medical name “Adhesive Capsulitis”. Read on to avoid common pitfalls when coping with the symptoms of frozen shoulder that could dramatically reduce your healing time.
Frozen Shoulder (Adhesive Capsulitis)
What is it?
Frozen shoulder (adhesive capsulitis) is a term that is used to refer to chronic inflammation categorised by pain and significantly reduced range of movement in the shoulder. Due to irritation, thickening and formation of scar tissue of the shoulder capsule which occurs over time, individuals can typically experience symptoms of frozen shoulder for anywhere from 6 months up to approximately 3.5 years.
Frozen shoulder is often characterised by it’s three over-lapping stages stages;
Stage one – Freezing (lasting approximately 3-9 months)
Stage two – Frozen (lasting approximately 4-12 months)
Stage three – Thawing (lasting approximately 1-3.5 years)
All of which bring their own set of symptoms and considerations.
Symptoms
As frozen shoulder is a chronic condition, individuals will typically complain of varying symptoms depending on the stage of injury.
Frozen stage: Gradual onset of pain and a gradual decrease in range of movement. Pain is typically sharp and worse at night. note
Freezing stage: As individual’s progress into the freezing stage, pain will begin to decrease however, further restrictions in range of movement will be experienced; often significantly reducing the persons ability to move their arm above 90 degrees. Pain is generally only felt at the end range of movement.
Thawing stage: During this stage a reduction in symptoms can be very spontaneous and individual’s typically feel a gradual improvement in their range of movement.
Causes
Primary causes of frozen shoulder remain largely unclear, however there are several predisposing factors that can lead to a greater risk of joint inflammation. These includes; females aged 40-65 years old due to hormonal changes in the body and individuals with diabetes or a weakened immune system.
Due to these risk factors; Individuals who have experienced a frozen shoulder have an increased chance of developing the condition in their opposite shoulder at some point.
Frozen Shoulder can also occur as the result of trauma to the shoulder joint or secondary to other shoulder conditions or injuries, due to the development of scar tissue within the joint causing stiff and rigid tissue. This can significantly impair range of movement around the shoulder joint.
Common Myths
A steroid injection will cure frozen shoulder – False!
Although in some case their may be a need for a steroid injection in the management of frozen shoulder, it is by no means a cure and is instead best use in combination with manual and exercise therapy to help control the symptoms of frozen shoulder by reducing inflammation.
Frozen shoulder only affects older women – False!
This is a common misconception of frozen shoulder and although females between the ages of 40-65 are at an increased risk of developing frozen shoulder, the condition can in fact also affect both men and people of a younger age and has been shown to be closely linked to being unhealthy in other ways such as smoking, sleep deprivation, and being out of shape.
How is it treated?
Although there is no magic cure, undertaking an exercise programme is imperative for recovery from Frozen Shoulder.
During the first stage of injury the main focus of treatment is to provide pain relief, any activities that provoke symptoms should be avoided and exercises that can be performed pain free have been shown to be the most beneficial. During the second stage of injury hands-on treatment is focused on trying to maintain range of movement and a greater range of pain free stretching exercises can be introduced. In the final phase of treatment, exercise progressions include the introduction of strengthening exercises in line with the restoration movement around the shoulder.
Common treatments to support an exercise programme include; gentle shoulder mobilisation, muscle release, manipulation, acupuncture and taping techniques.
In very extreme cases of frozen shoulder, the shoulder joint can undergo a procedure know as manipulation under anaesthetic (MUA).
What Can You Do?
Developing a comprehensive understanding of Frozen Shoulder will help you to understand what symptoms you can expect during the different stages of injury.
Application of heat to encourage muscle relaxation and extensibility is advised particularly within the initial stage of injury.
Avoiding any activities or movement that reproduces the pain will help you to manage your daily symptoms.
Reducing the risk of other unhealthy contributors such as reducing or cutting out smoking, increasing sleep and maintaining a healthy diet.
If you know anyone that the information in this article could help, then please feel free to pass it on and share with your family and friends.